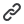Employer Sponsored Health Coverage Explained
The Affordable Care Act, also known as Obamacare, is simpler than some people may give it credit for. Employers with 50 full-time employees or more are obligated to sponsor plans for their workers to help them meet this requirement.
The One Big Beautiful Bill that passed includes permanently extending tax cuts from the Tax Cuts and Jobs Act, including increasing the cap on the amount of state and local or sales tax and property tax (SALT) that you can deduct, makes cuts to energy credits passed under the Inflation Reduction Act, makes changes to taxes on tips and overtime for certain workers, reforms Medicaid, increases the Debt ceiling, and reforms Pell Grants and student loans. Updates to this article are in process. Check our One Big Beautiful Bill article for more information.
Key Takeaways
- According to the Affordable Care Act, the premiums you pay to an employer-sponsored health plan for your own coverage can't exceed 8.39% of your 2024 household income.
- If you add coverage for other members of your family, the premiums may exceed 8.39% of your household income.
- If your share of the health insurance premiums through your employer is more than 8.39% of your 2024 income, you can get health insurance through the Health Insurance Marketplace.
- If the premiums for your employer-sponsored health insurance are equal to or less than 8.39% of your 2024 income, you can’t claim the premium tax credit if you buy through the Marketplace instead.
What is employer-sponsored coverage?
The first step in understanding employer-sponsored health coverage is figuring out whether you have it. Technically, a health plan can be offered by your employer, available within your state or sponsored by the government.
If you purchase insurance privately or through the Health Insurance Marketplace, this isn’t employer-sponsored coverage. But if you’re covered by a health plan provided through your job, it’s most likely employer-sponsored. Check with human resources or your boss to be sure.
Premiums must be affordable
“The new health care law says that your contributions to a health plan sponsored by your employer must be affordable for you,” says Chip Capelli, an accountant with offices in Philadelphia and Provincetown, Massachusetts. Your definition of affordable might be different from your employer’s so the law includes specific guidelines for 2024:
- Premiums can’t exceed 8.39% of your household’s income after taking your employer’s contributions into the equation.
- Technically, this means that if both you and your spouse work, the 8.39% applies to your combined incomes.
But as a practical matter, many employers just go by the income reported on your W-2, because they have no way of identifying exactly what your household’s income might be.
What does affordable coverage mean to you?
If your share of the health insurance premiums through your employer is more than 8.39% of your 2024 income, you can get health insurance through the Health Insurance Marketplace, the website where you can get coverage when a more affordable plan isn’t available to you. When this is the case, you are likely eligible for the Premium Tax Credit to help pay the cost.
But if your employer offers health insurance that is equal to or less than 8.39% of your 2024 income, you can’t claim the premium tax credit if you buy through the Marketplace instead, a choice you might make if purchasing a policy there would be less expensive or offers better coverage than your employer-sponsored options.
TurboTax Tip:
If you decline employer-sponsored coverage, you can’t take advantage of the Premium Tax Credit if you buy in the Marketplace instead, no matter what your reasons.
There’s a family affordability glitch
Some taxpayers fall into what’s being called a “family affordability glitch.” The affordability rule applies only to coverage for you, not for your dependents. So, when you add on coverage for your entire family, the premiums may exceed 8.39% of your 2024 income.
If you decline employer-sponsored coverage, you’ll still be barred from taking advantage of the Premium Tax Credit if you buy in the Marketplace instead, no matter what your reasons.
Non-complying Applicable Large Employers (ALEs) may pay fines
It’s likely in your employer’s best financial interests to offer you coverage you can afford. “The government encourages employers to offer affordable health care coverage by imposing some stiff monetary fines when they don’t,” says Capelli.
For 2024, if even one of a company’s workers receives a premium tax credit through the Marketplace because the company’s health insurance plans don’t meet the law’s standard for affordability, the employer must pay an annualized penalty equal to $4,460 multiplied by the number of employees who receive the premium tax credit.
- If 10 of them receive a premium tax credit, this amounts to a $44,600 fine (10 x 4,460)
But this isn’t as steep as the fine a company faces if it employs more than 50 workers and offers no employer-sponsored health coverage at all.
- The fine in 2024 is $2,970 per employee, less 30 employees.
- For example, if the company employees 75 full-time workers, the fine would be:
o 75 – 30 = 45 employees
o 45 x $2,970 = $133,650 fine
With TurboTax Live Full Service, a local expert matched to your unique situation will do your taxes for you start to finish. Or get unlimited help and advice from tax experts while you do your taxes with TurboTax Live Assisted.
And if you want to file your own taxes, TurboTax will guide you step by step so you can feel confident they'll be done right. No matter which way you file, we guarantee 100% accuracy and your maximum refund.
Get started now by logging into TurboTax and file with confidence.